29. Full Mouth Rehabilitation: Restoring Mandibular Position and Occlusal Balance
Case Summary
A male patient in his 50s presented with significant functional and aesthetic concerns stemming from a long-term collapsed occlusion. Due to years of wearing dentures with an insufficient vertical dimension (low VDO), the patient experienced a "domino effect" of oral health issues:
Mandibular Retrusion & Deep Bite: The lack of posterior height caused the mandible to shift backward, creating a pathological deep bite.
Anterior Pathological Migration: Without stable posterior "stops," excessive occlusal forces were transferred to the anterior segment, leading to labial flaring and the development of wide diastemas (spacing).
Functional Instability: The patient suffered from reduced masticatory efficiency and an unpredictable bite relationship.
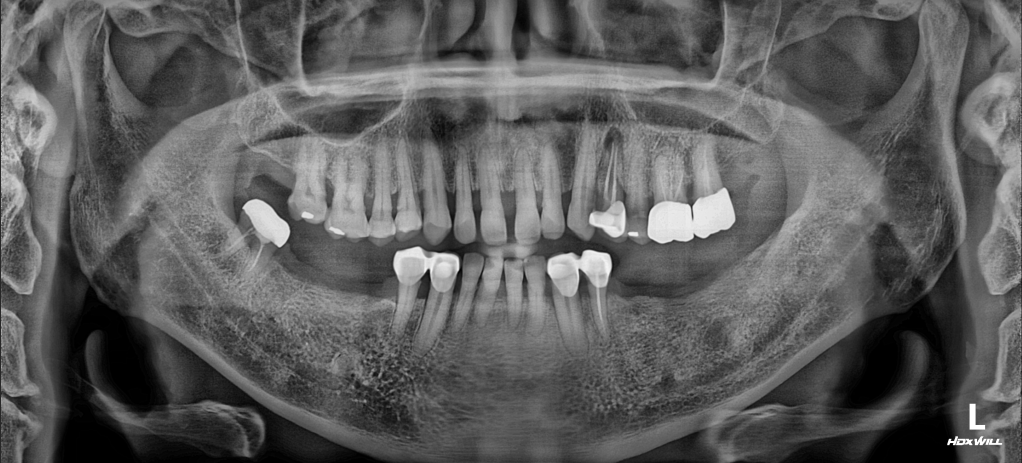
OPG - BEFORE
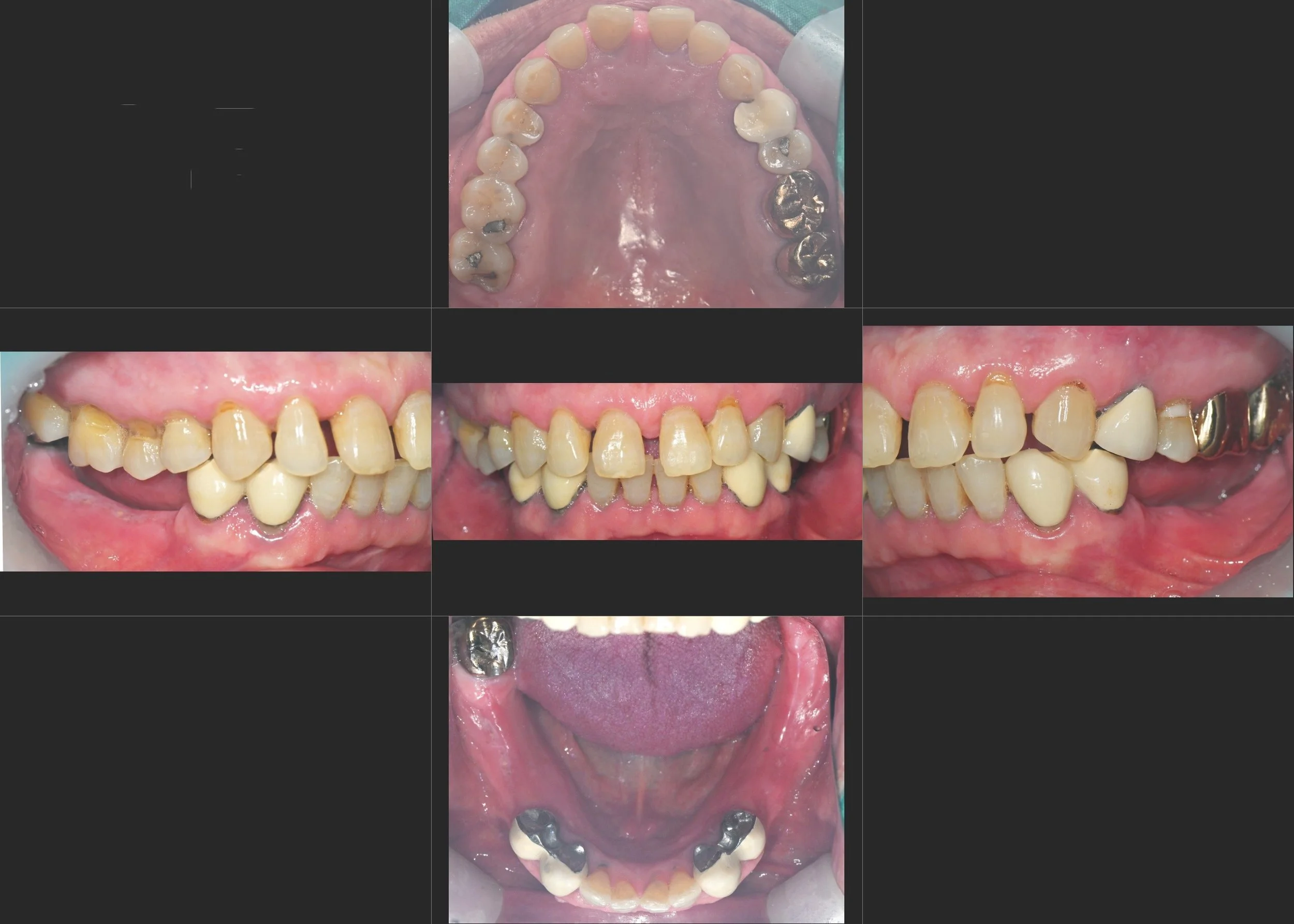
INTRA ORAL - BEFORE
Treatment Objectives
VDO Recovery: To re-establish the lost vertical dimension and provide adequate restorative space.
Mandibular Repositioning: To guide the mandible forward into a more physiologically neutral and stable position.
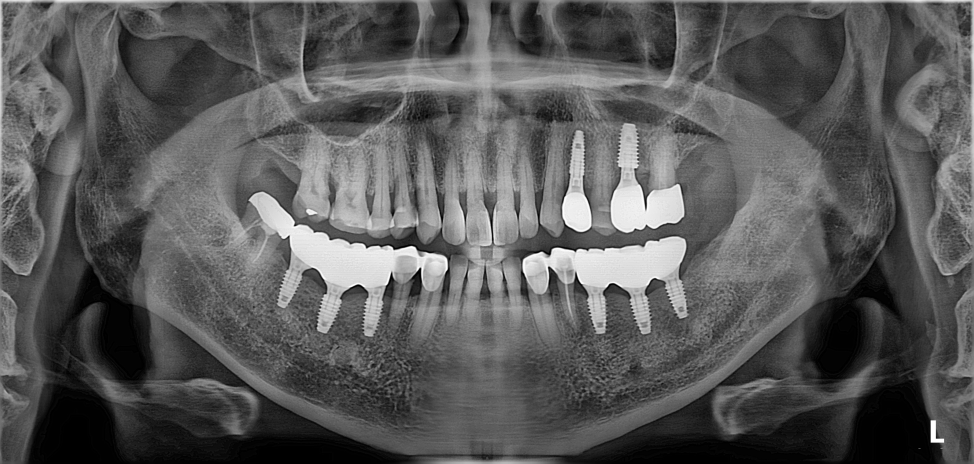
Stable Posterior Support: To place dental implants in the posterior segments, creating a firm foundation for the new occlusion.
Minimally Invasive Aesthetic Correction: To close anterior spaces and correct the flaring effect using non-prep veneers (laminates), preserving maximum natural tooth structure.
Predictable Force Balance: To achieve a harmonious distribution of occlusal forces to ensure long-term prosthetic success.
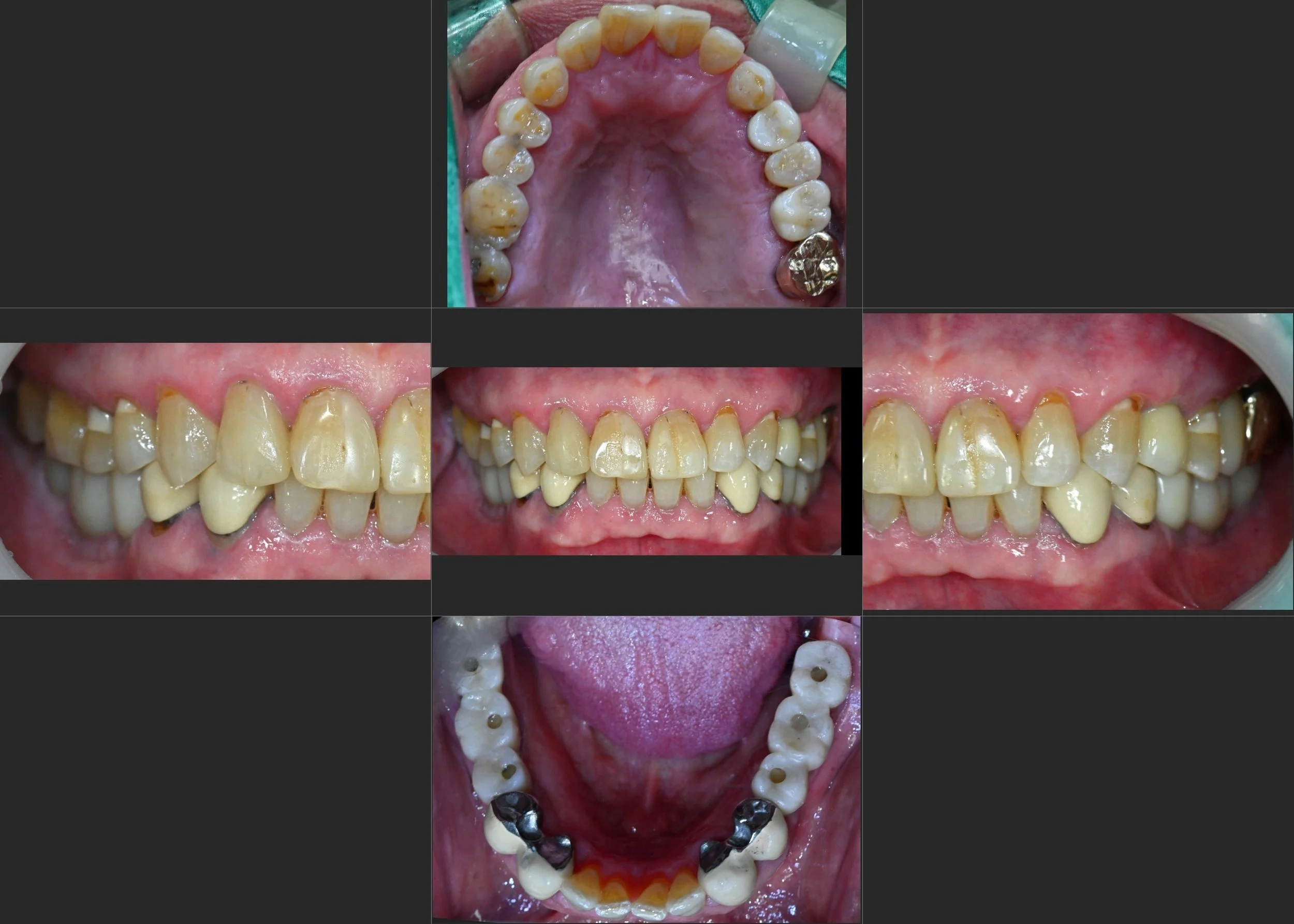
INTRA ORAL - AFTER
Treatment Approach
The rehabilitation was focused on transitioning the patient from a pathological state to a state of "predictable balance":
Phase 1: Posterior Stabilization: Dental implants were strategically placed in the posterior regions. These units served as the primary anchors for the new VDO, effectively "unlocking" the mandible from its retruded position.
Phase 2: Adaptation & Guidance: During the provisional phase, the patient's adaptation to the new occlusal height and mandibular position was carefully monitored. This ensured that the neuromuscular system was in harmony with the proposed final restorations.
Phase 3: Anterior Refinement (Non-prep): Once the posterior stability was confirmed, the anterior spacing was addressed. To honor the patient's biological integrity, non-prep ceramic veneers were utilized. This approach allowed us to close the flared gaps and restore a youthful smile line without unnecessary tooth reduction.
Final Occlusal Calibration: The final restorations were delivered with a focus on mutual protection, ensuring that the posterior implants bear the load of mastication while the anterior veneers provide aesthetic harmony and proper guidance.
The result is a functional and aesthetic transformation that not only restored the patient's smile but also found the "sweet spot" of occlusal equilibrium.