23. Restoring Function and Trust: Comprehensive Full-Mouth Rehabilitation
Case Summary
A male patient in his 60s presented with a severely compromised dentition and significant psychological barriers. Due to past negative dental experiences, he harbored a deep distrust of dental treatment, which led to years of neglect.
The primary clinical findings included:
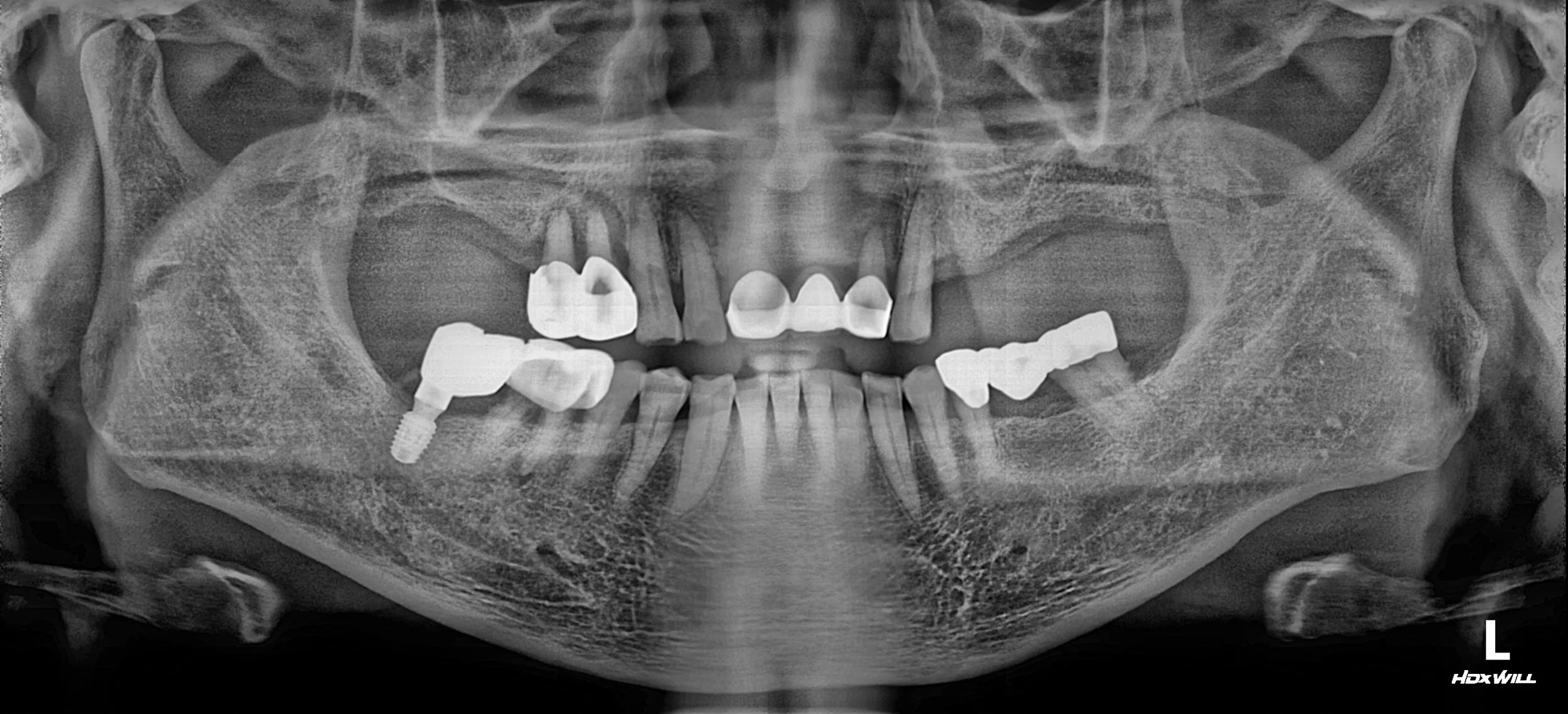
Posterior Bite Collapse: Loss of posterior support resulting in a reduced Vertical Dimension of Occlusion (VDO).
Pathological Anterior Flaring: Without posterior stops, excessive forces caused the maxillary anterior teeth to drift labially (flaring), creating aesthetic and functional distress.
Failing Prosthetics & Periodontitis: Existing restorations were ill-fitting, and generalized periodontal disease had further destabilized the remaining teeth.
OPG - BEFORE
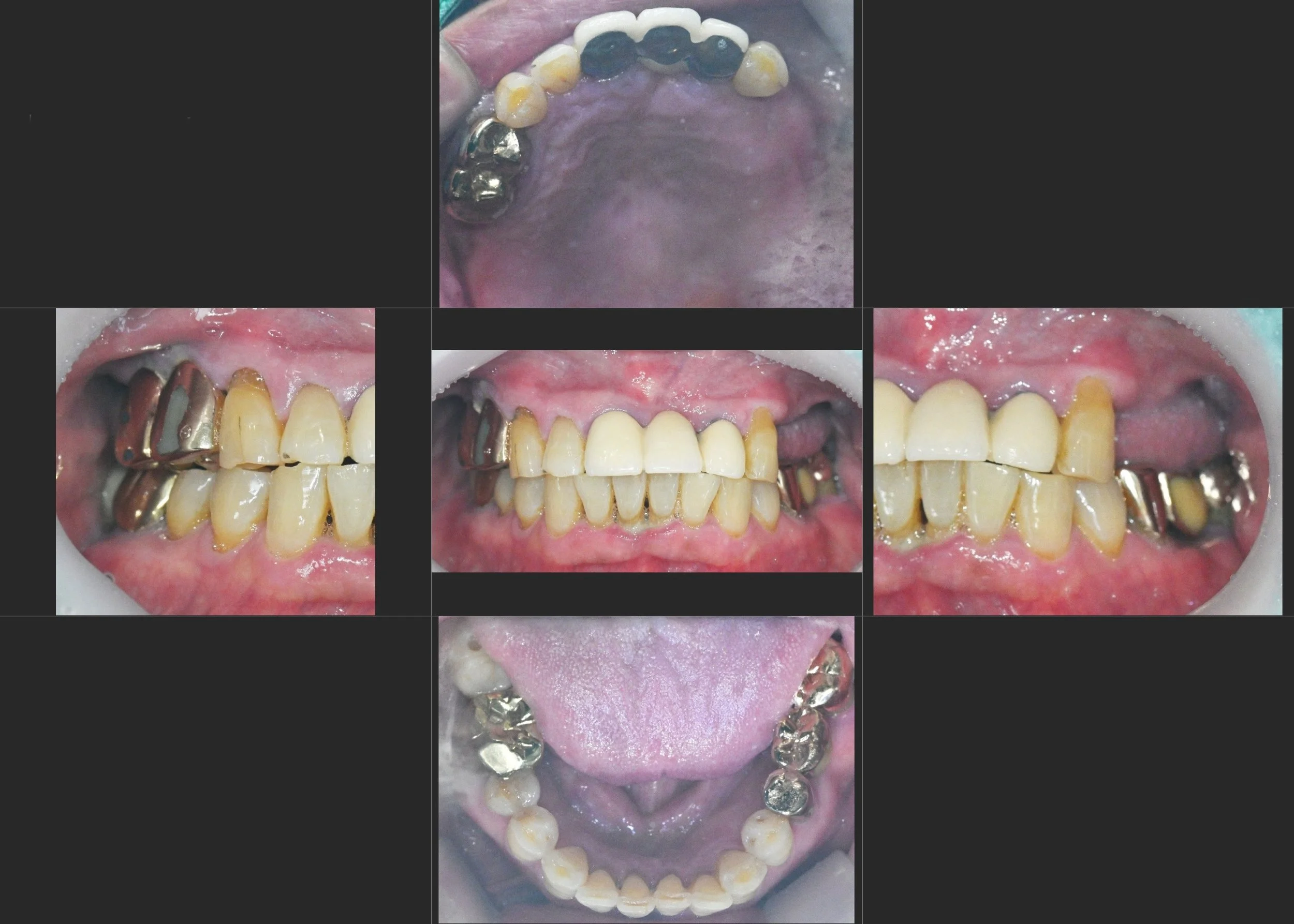
INTRA ORAL - BEFORE
Treatment Objectives
Trust Building: To establish a predictable treatment environment through transparent communication and phased success.
VDO Elevation: To recover the lost vertical dimension and provide space for both functional and aesthetic reconstruction.
Periodontal Management: To stabilize the supporting tissues through comprehensive periodontal therapy before final restoration.
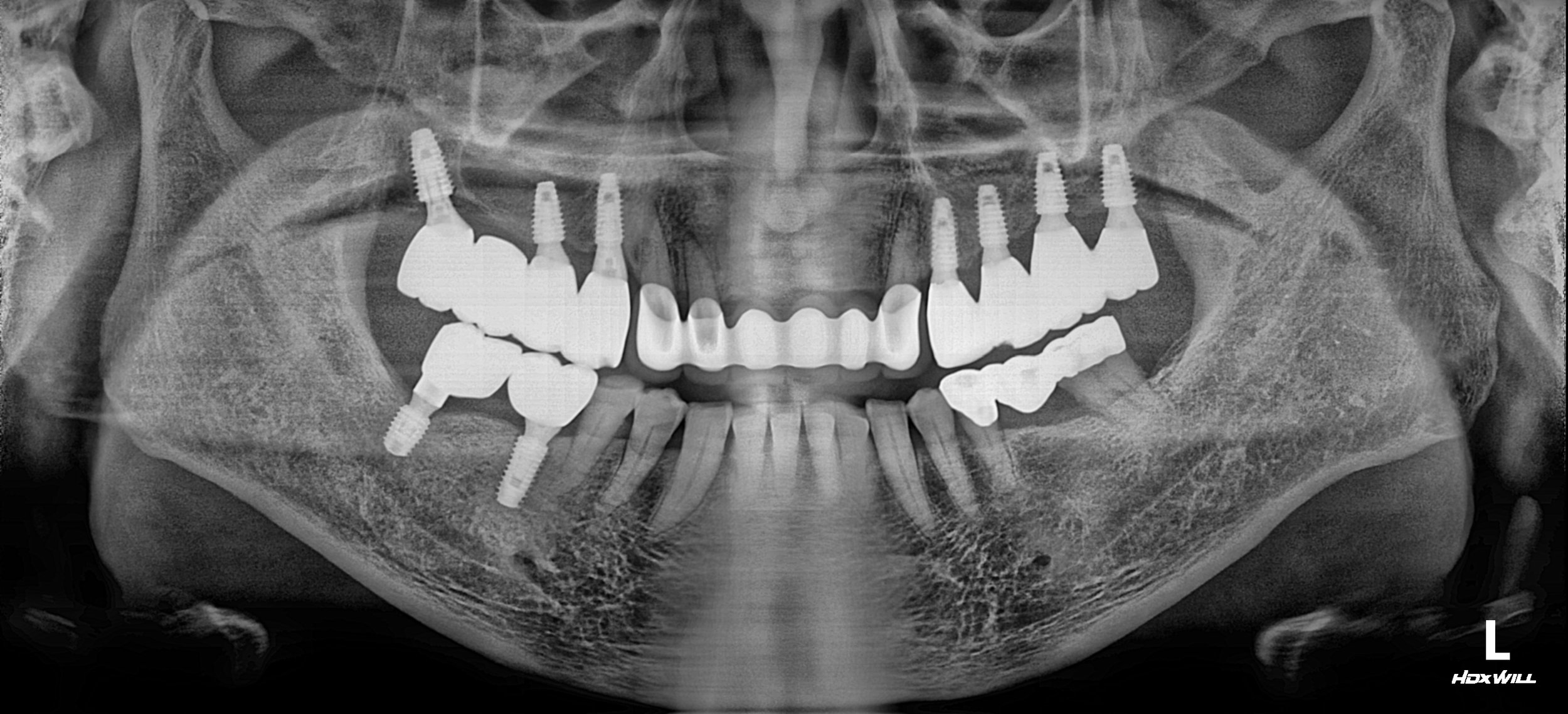
Occlusal Stabilization: To place posterior implants and replace failing crowns to create a stable, repeatable centric relation.
Anterior Realignment: To correct the flaring effect and restore the anterior smile line.
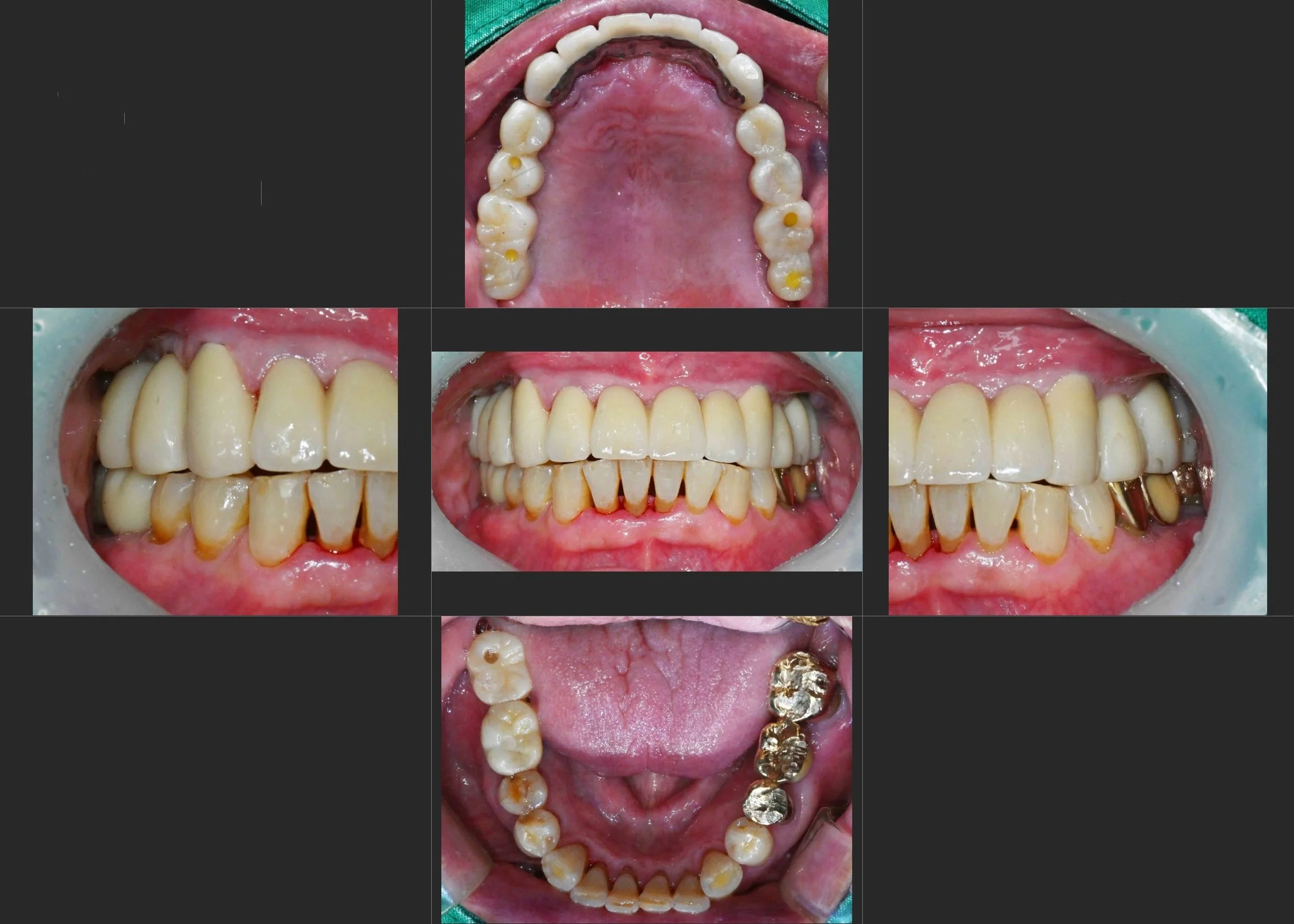
INTRA ORAL - AFTER
Treatment Approach
The treatment was executed with a "stability-first" philosophy to manage both the clinical complexity and the patient's anxiety:
Periodontal & Preliminary Phase: The journey began with thorough periodontal treatment and the removal of hopeless restorations. This phase was crucial for demonstrating clinical progress and building the patient's trust.
VDO Elevation & Implant Surgery: Dental implants were placed in the posterior edentulous areas. Simultaneously, the VDO was elevated using long-term provisional restorations. This "trial occlusion" allowed the patient to adapt to the new bite height and monitored for any TMJ discomfort.
Occlusal Stabilization Period: We maintained the patient in a stabilized temporary state for several months. This period ensured that the new posterior support was robust and the mandibular position was consistent before touching the aesthetic zone.
Final Aesthetic Restoration: Once occlusal stability was confirmed, the anterior teeth were restored. By resetting the occlusion, we were able to eliminate the flaring forces, providing a natural and stable anterior relationship.
The patient, who initially approached treatment with extreme skepticism, is now functioning with full confidence and expresses high satisfaction with both the comfort of his bite and the rejuvenation of his smile.