33. Comprehensive Revision Therapy: Reclaiming Function from Multiple Implant Failures
Case Summary
A male patient in his 50s presented with multiple failing dental implants in the maxillary arch. The clinical situation was critical, characterized by:
Failing and Lost Implants: Previous implants were non-functional or had been removed due to severe peri-implantitis and bone loss.
Severe Alveolar Resorption: The supportive bone was highly compromised, both horizontally and vertically, particularly in the failing segments.
Soft Tissue Atrophy: A lack of attached gingiva and shallow vestibule complicated future maintenance and prosthetic success.
Occlusal Disharmony: With no stable posterior stops, the patient had completely lost functional occlusal balance.
A comprehensive revision plan was required, focusing on both the foundation (bone and soft tissue) and the function (occlusal stability).
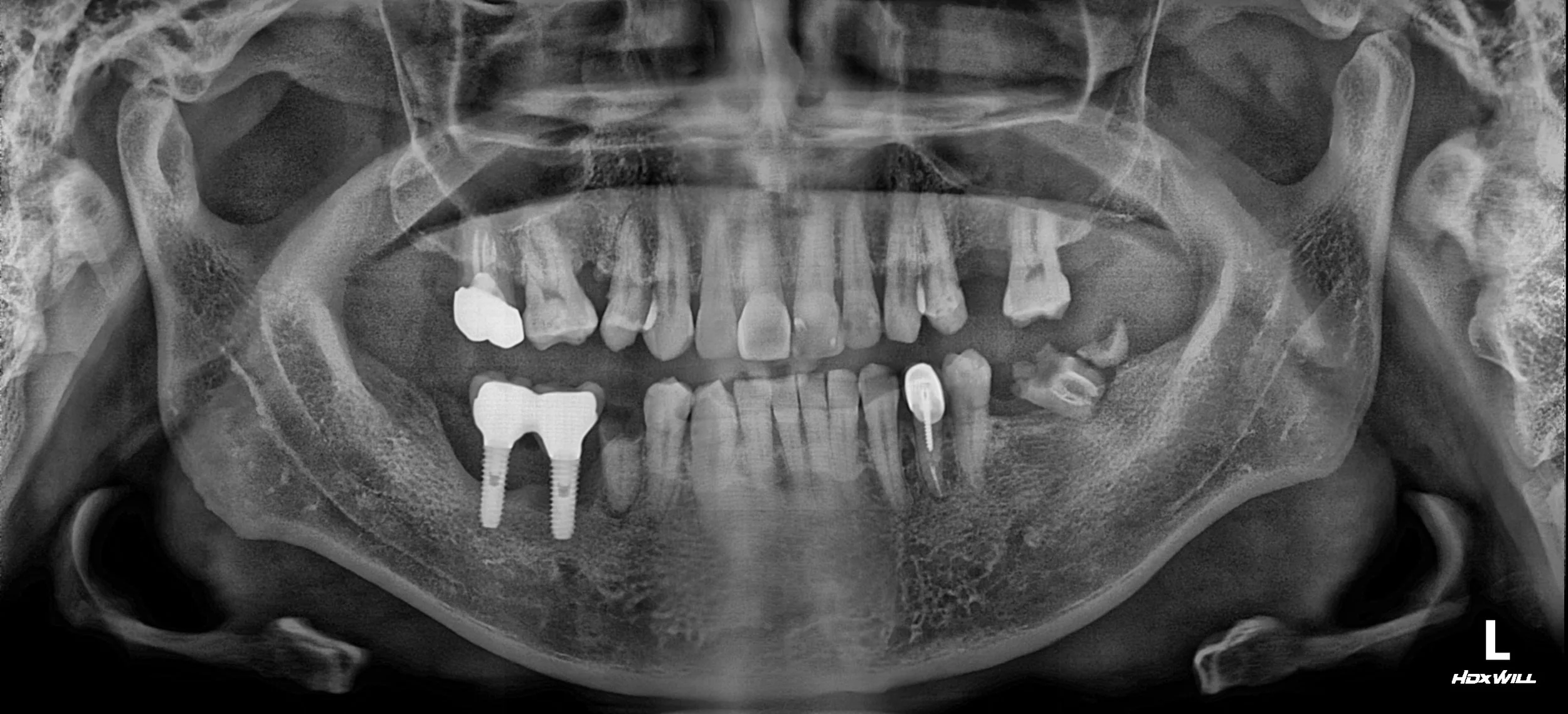
OPG - BEFORE
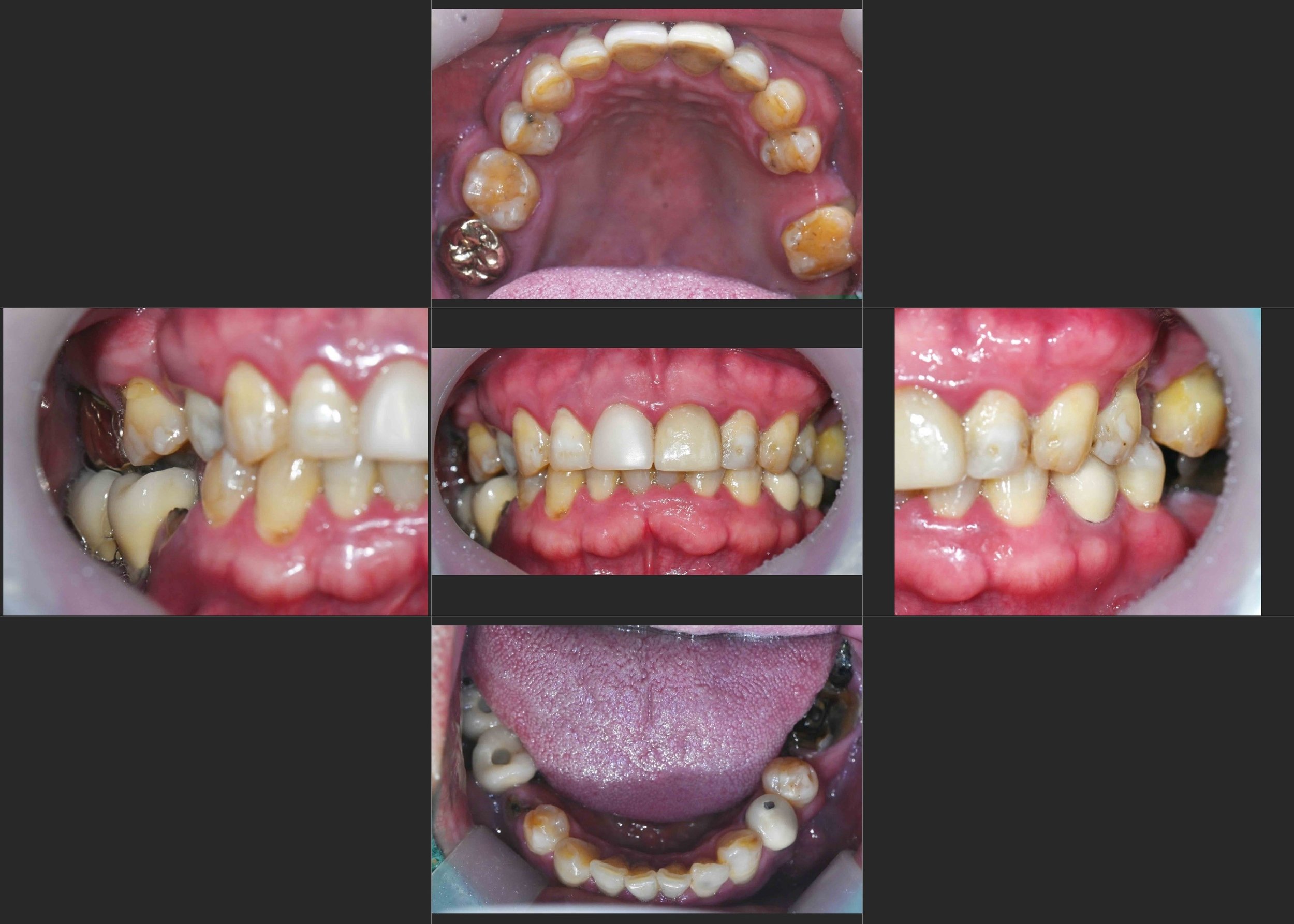
INTRA ORAL - BEFORE
Treatment Objectives
Foundation Reconstruction (GBR): To perform extensive Guided Bone Regeneration (GBR) to rebuild the alveolar ridge for stable implant placement.
Soft Tissue Revision (Vestibuloplasty): To perform a vestibuloplasty to deepen the vestibule and increase the zone of attached gingiva, facilitating long-term peri-implant maintenance and prosthetic comfort.
Functional Synchronization: To re-establish a stable vertical dimension (VDO) and harmonious centric relation (CR) using extended provisional guidance.
Sustainable Occlusion: To convert a high-risk, failing occlusal state into a predictable, fixed rehabilitation.
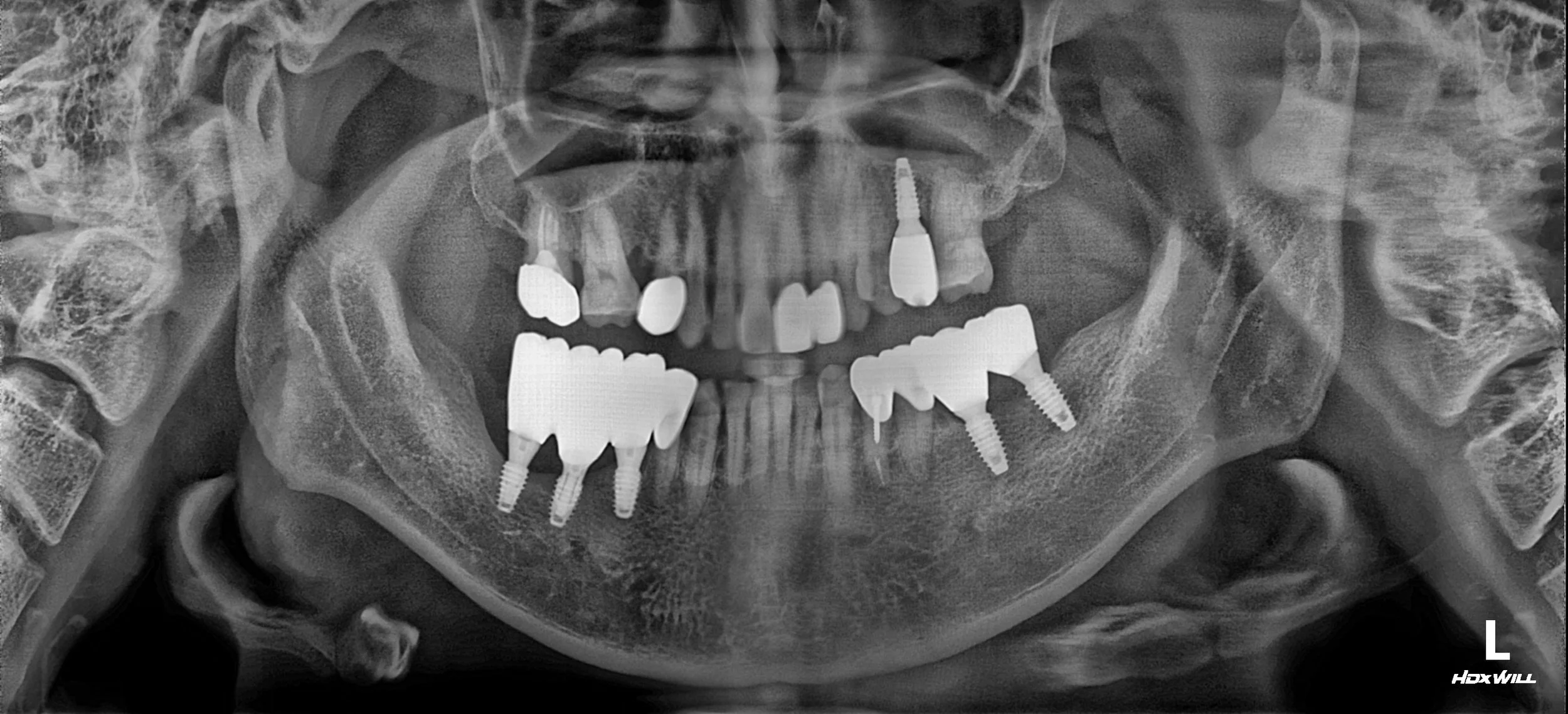
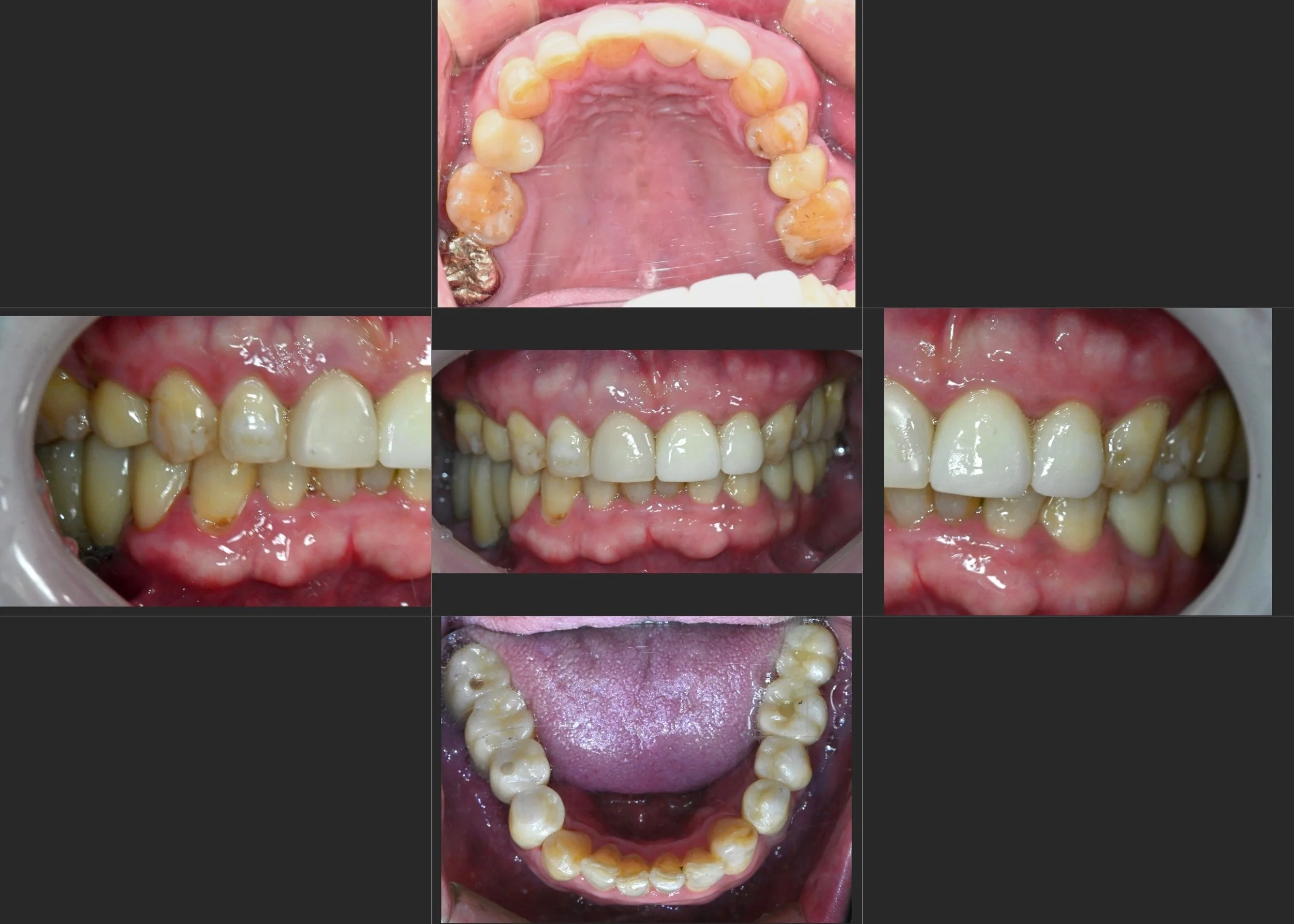
INTRA ORAL - AFTER
Treatment Approach
The rehabilitation was managed through a structured, multi-phase protocol to manage the severe foundational and functional challenges:
Initial Debridement & Removal: Non-restorable failing implants and hopeless teeth were removed. This phase was crucial for eradicating infection and stabilizing the periodontal foundation.
Surgical Phase (Hard & Soft Tissue): Simultaneous or staged Guided Bone Regeneration (GBR) was performed to address severe bone atrophy. Following initial healing, a vestibuloplasty was conducted to deepen the vestibule and improve the soft tissue quality for long-term health.
Prosthetic Revision & Functional Phase: Dental implants were strategically re-placed at the intended new VDO. This phase was meticulously planned to prevent future overloading and to harmonize with the new mandibular position. Comprehensive functional guidance was initiated using long-term provisional restorations. The patient was maintained in this stabilized temporary state for an extended period, allowing the neuromuscular system to fully adapt and ensuring the new bite position was repeatable and comfortable.
Final Prosthetic Phasing: Definitive zirconia implant-supported bridges were delivered. Particular attention was paid to creating a harmonious "emergence profile" for maintenance. The final occlusal scheme was designed to be "maintenance-friendly," ensuring easy access for hygiene, vital for patients with a history of severe failures.
The result is a transformative improvement, moving from the discomfort of iatrogenic failure and skeletal collapse to a stable, functional, and symmetrical fixed rehabilitation.