35. Comprehensive Full-Arch Transformation: Restoring Confidence in a Young Phobic Patient
Case Summary
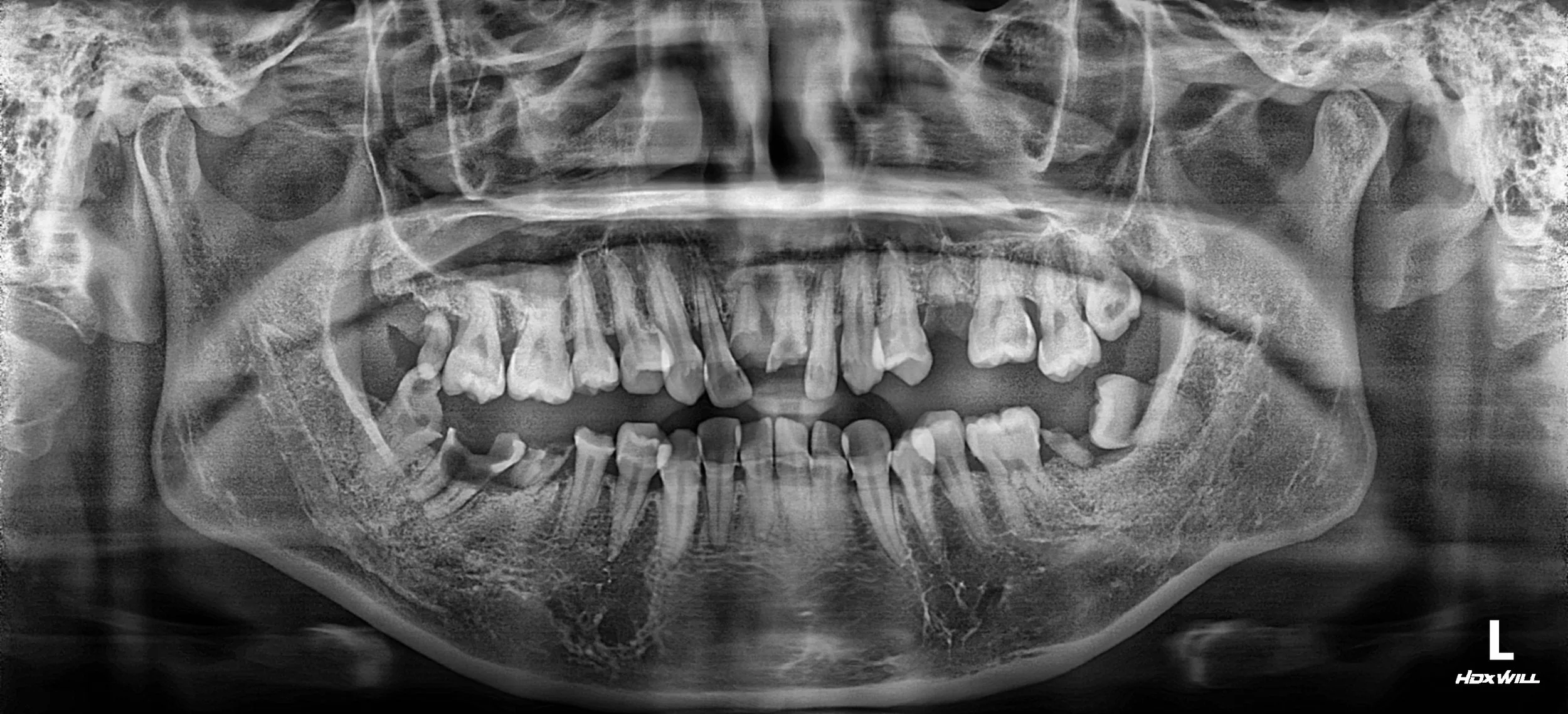
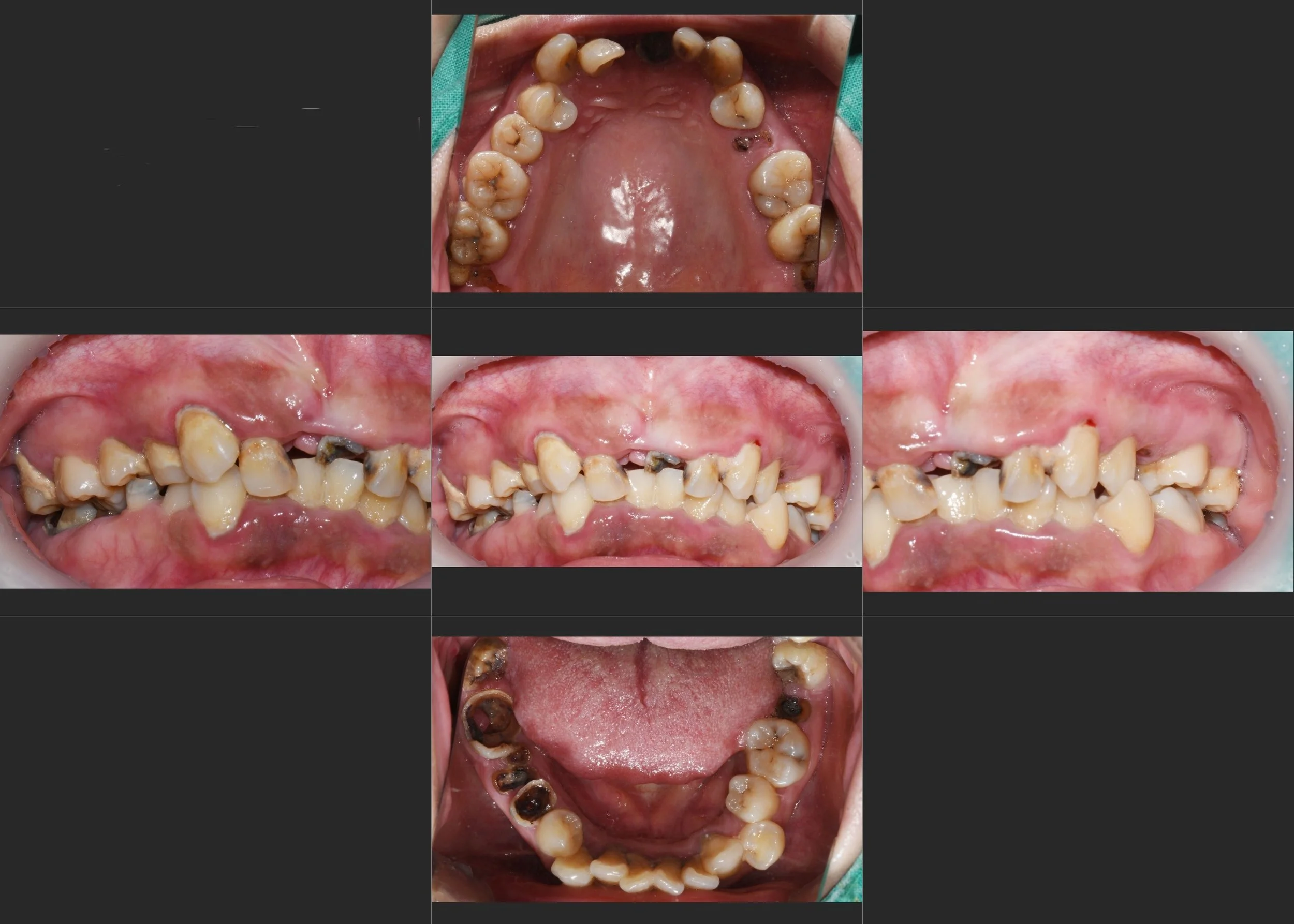
A female patient in her 20s presented with a severely compromised dentition and profound psychological distress. Generalized rampant caries had decimated her remaining teeth, resulting in a completely collapsed occlusion and non-restorable roots throughout both arches.
Due to severe dental phobia, the patient had neglected treatment for years, which had significant psychosocial consequences. She was unable to speak or smile comfortably, constantly wore a face mask, and was suffering from increasing social avoidance.
OPG - BEFORE
INTRA ORAL - BEFORE
Treatment Objectives
Psychological Management: To establish a comfortable treatment environment to help the patient overcome her severe dental phobia.
Preservation Strategy: To perform necessary periodontal and endodontic therapy on salvageable teeth, preserving them as abutments where clinically viable.
Strategic Implant Placement: To place dental implants in the edentulous posterior areas to provide the robust support needed for a balanced occlusion.
VDO Elevation: To recover the lost vertical dimension and stabilize the intermaxillary relationship.
Aesthetic Rehabilitation: To provide naturally aesthetic, full-arch prosthetics, allowing the patient to regain her social confidence.
Maintenance Protocol: To establish a strict 3-month maintenance recall system with detailed, personalized oral hygiene education.
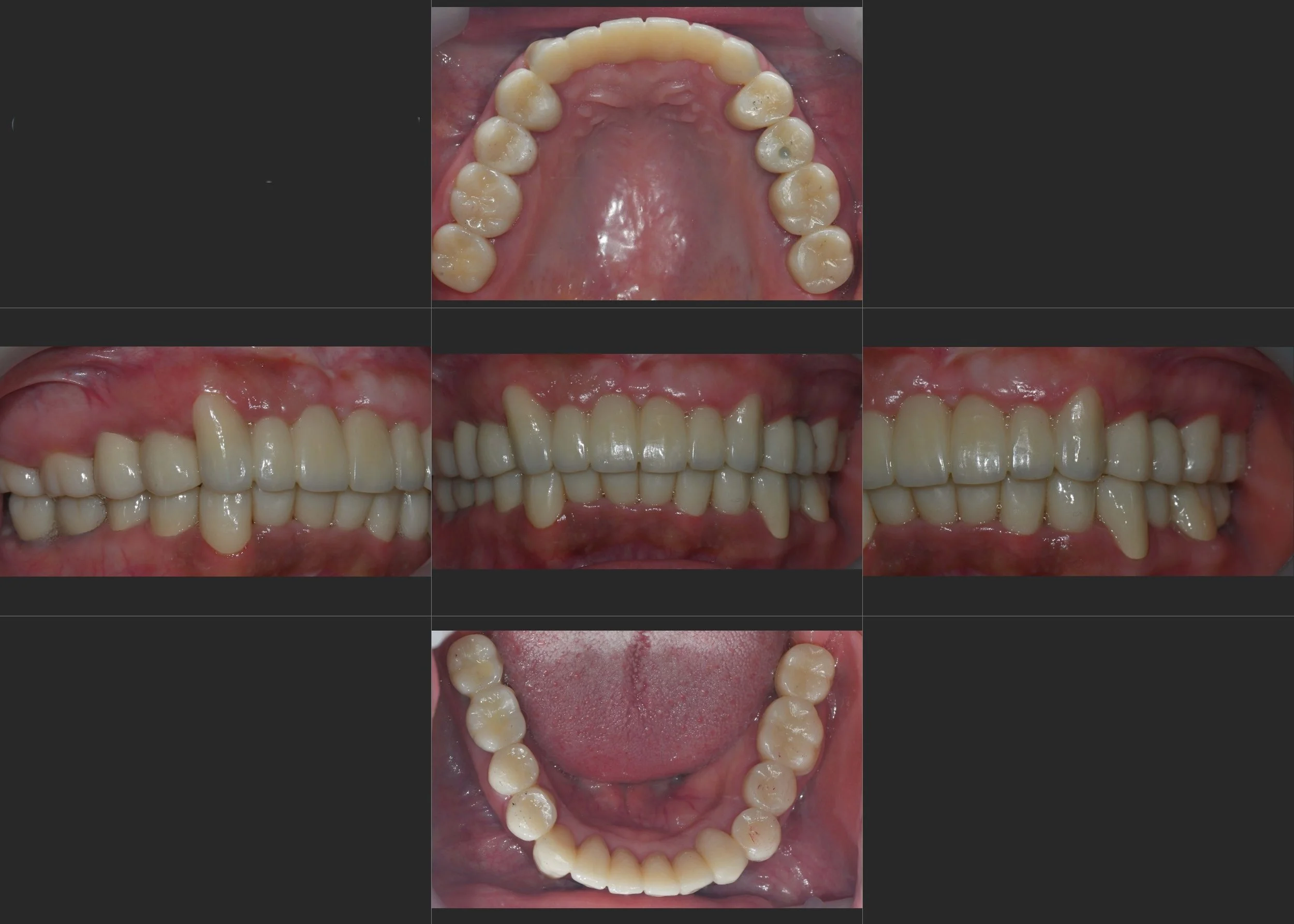
INTRA ORAL - AFTER
Treatment Approach
The treatment was conducted in phases to accommodate the patient's anxiety and the complexity of the reconstruction:
Initial Stabilization & Education: Priority was placed on controlling active infection and building the patient's trust. detailed oral hygiene instruction was initiated immediately, emphasizing the necessity of self-care.
Tooth Preservation & Endodontics: Prioritizing infection control, endodontic therapy was performed on salvageable teeth. Hopeless teeth were extracted.
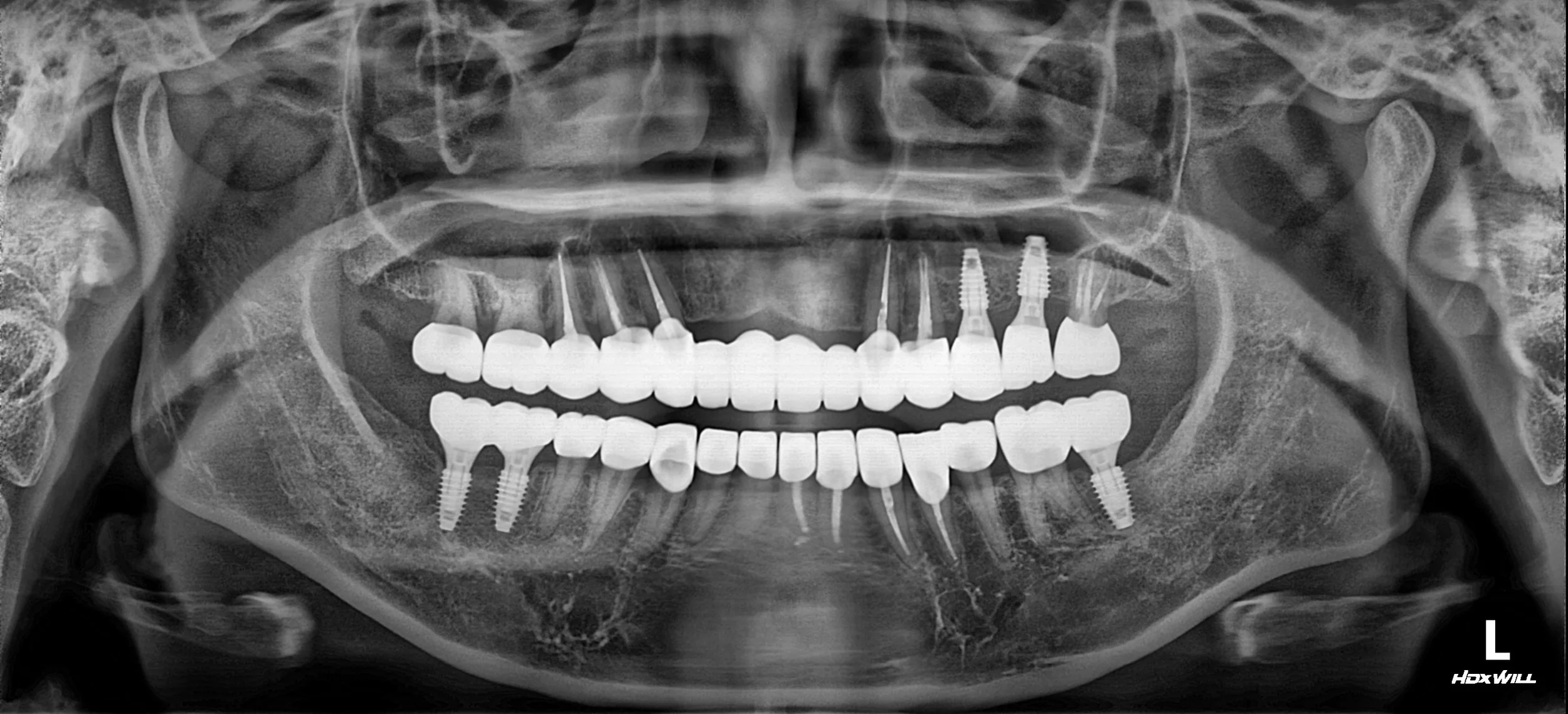
VDO Management & Implant Surgery: The vertical dimension of occlusion (VDO) was reset to a more physiologically neutral height. Temporaries were used to stabilize the bite. Following GBR, strategically placed implants were integrated into the posterior edentulous regions to serve as the primary occlusal stops.
Prosthetic Integration: Precision-milled fixed bridges were fabricated. A combination of tooth-supported and implant-supported restorations was used to achieve a harmonious and balanced occlusal scheme.
Strict Maintenance Program: Final delivery was accompanied by meticulous oral hygiene instruction. Given the history of neglect, the patient was enrolled in a personalized maintenance program with regular 3-month recall appointments to ensure long-term stability and health.
The final transformation allowed the patient to fully regain her ability to smile without hesitation, marking the end of her fear of dental care and her need to hide behind a mask socially.